Digital Health Course, Autumn Semester 2019, University of St.Gallen

NHS teams up with Amazon to bring Alexa to patients (The Guardian, July 2019), Contactless cardiac arrest detection using smart devices (Nature Digital Medicine, June 2019), Apple Heart Study demonstrates ability of wearable technology to detect atrial fibrillation (StandfordMedicineNews, March 2019),Digital health companies raised a total of $4.2B across 180 deals through the first half of 2019. If this pace holds steady, the sector is on track for an $8.4B year in 2019 – and may even top 2018’s record-breaking annual funding total. Sean Day, Rocket Health, 2019 Midyear Digital Health Market Update
What are the rationale and implications behind the recent developments in the field of digital health?
Digital Health is the use of information and communication technology for the prevention and treatment of diseases in the everyday life of individuals. It is thus linked to topics such as digital health interventions, digital biomarker, digital coaches and healthcare chatbots, telemedicine, mobile and wearable computing, self-tracking, personalized medicine, connected health, smart homes or smart cars.
In the 20th century, healthcare systems specialized in acute care. In the 21st century, we now face the challenge of dealing with the specific characteristics of chronic conditions. These are now responsible for around 70% of all deaths worldwide and 85% of all deaths in Europe and are associated with an estimated economic loss of $7 trillion between 2011 and 2025. Chronic diseases are characterized in particular by the fact that they require an intervention paradigm that focuses on prevention and lifestyle change. Lifestyle (e.g., diet, physical activity, tobacco or alcohol consumption) can reduce the risk of suffering from a chronic condition or, if already present, can reduce its burden. A corresponding change in lifestyle is, however, only implemented by a fraction of those affected, partly because of missing or inadequate interventions or health literacy, partly due to socio-cultural influences. Individual personal coaching of these individuals is neither scalable nor financially sustainable.
Against this background, the question arises on how to develop evidence-based digital health interventions (DHIs) that allow medical doctors and other caregivers to scale and tailor long-term treatments to individuals in need at sustainable costs. At the intersection of health economics, information systems research, computer science, and behavioral medicine, this lecture has the objective to help students and upcoming healthcare executives interested in the multi-disciplinary field of digital health to better understand the need, design, and assessment of DHIs.
After the course, students will be able to…
- understand the importance of DHIs for the management of chronic conditions
- understand the anatomy ofDHIs
- know frameworks for the design ofDHIs
- know evaluation criteria forDHIs
- know technologies forDHIs
- assessDHIs
- discuss the advantages and disadvantages of DHIs
To reach these learning objectives, the following topics are covered in the lecture and will be discussed based on concrete national and international examples including DHIs from the Center for Digital Health Interventions (www.c4dhi.org), a joint initiative of the Department of Management, Technology and Economics at ETH Zurich and the Institute of Technology Management at the University of St.Gallen:
1. Motivation for Digital Health
- The rise of chronic diseases in developed countries
- The discrepancy of acute care and care of chronic diseases
- Lifestyle as medicine and prevention
- From excellence of care in healthcare institutions to excellence of care in everyday life
2. Anatomy of Digital Health Interventions
- Just-in-time adaptive interventions
- Digital biomarker for predicting states of vulnerability
- Digital biomarker for predicting states of receptivity
- Digital coaching and healthcare chatbots
3. Design & Evaluation of Digital Health Interventions
- Overview of design frameworks
- Preparation of DHIs
- Optimization of DHIs
- Evaluation of DHIs
- Implementation of DHIs
4. Digital Health Technologies
- Technologies for telemedicine
- Mobile medical devices
- Virtual, augmented and mixed reality applications incl. live demonstrations
- Privacy and regulatory considerations
Course structure
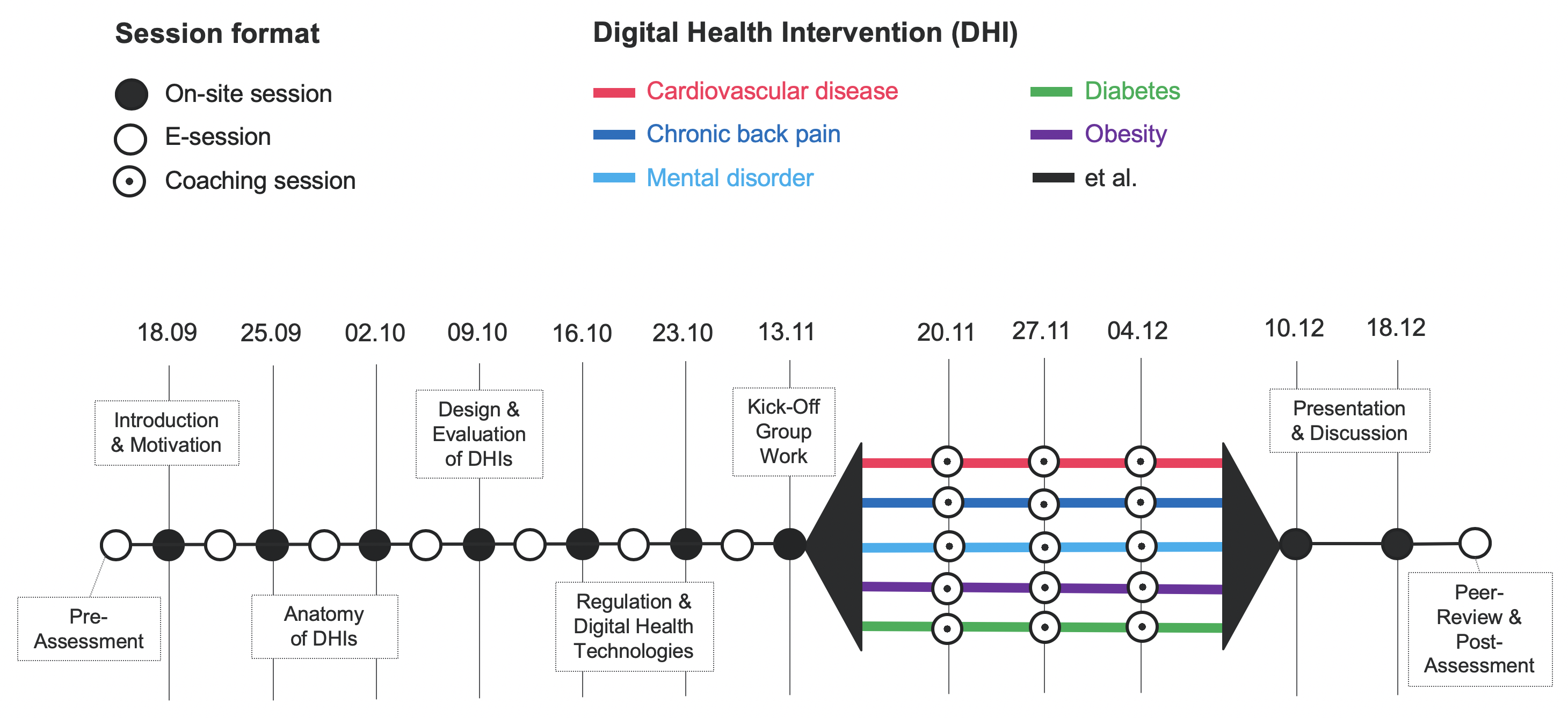
The Digital Health lecture is structured in two parts and follows the concept of a hybrid therapy consisting of on-site sessions and complementary online lessons. In the first part, students will learn and discuss the topics of the four learning modules in weekly on-site sessions. Complementary learning material (e.g., video and audio clips), multiple-choice questions and exercises are provided online.
In the second part, students work in teams and will use their knowledge from the first part of the lecture to critically assess DHIs. Each team will then present and discuss the findings of the assessment with their fellow students who will provide peer-reviews. Additional on-site coaching sessions are offered to support the teams with the preparation of their presentations.
Course literature
- Chaix, B. (2018) Mobile Sensing in Environmental Health and Neighborhood Research Annual Review of Public Health (39), 367-384.
- Collins, M. (2018) Optimization of Behavioral, Biobehavioral, and Biomedical Interventions: The Multiphase Optimization Strategy (MOST) New York:Springer.
- Corneta, P. and R.J. Holden (2018) Systematic Review of Smartphone-Based Passive Sensing for Health and Wellbeing Journal of Biomedical Informatics (77:January), 120-132.
- Coravos, A., Khozin, S. and K.D. Mandl (2019) Developing and Adopting Safe and Effective Digital Biomarkers to Improve Patient Outcomes Nature Digital Medicine 2 Paper14.
- Katz, L., E.P. Frates, J.P. Bonnet, S.K.Gupta, E. Vartiainen and R.H. Carmona (2018) Lifestyle as Medicine: The Case for a True Health Initiative American Journal of Health Promotion 32 (6),1452-1458.
- Kvedar, C., A.L. Fogel, E. Elenko and D.Zohar (2016) Digital medicine’s march on chronic disease NatureBiotechnology 34 (3), 239-246.
- Nahum-Shani, I., S. N. Smith, B. J. Spring, L. M. Collins, K. Witkiewitz, A. Tewari and S. A. Murphy (2018) Just-in-Time Adaptive Interventions(JITAIs) in MobileHealth: Key Components and Design Principles for Ongoing Health Behavior Support Annals of Behavioral Medicine 52 (6),446-462.
Mandatory material
The mandatory material will be provided via the online learning platform.
Additional course information
This lecture builds the foundation for the Digital Health Project seminar offered in the spring semester 2020. In that seminar, teams of students will develop a smartphone-based digital health intervention with MobileCoach (www.mobile-coach.eu), an open-source platform for digital health interventions and ecological momentary assessments with the support of the Center for Digital Health Interventions (www.c4dhi.org).
Summary
Digital Health, University of St.Gallen, Autumn Semester 2019, 7,800, 3 ECTS credits, Building 23, Room 23-201, Wednesday, 4:15 p.m. – 5:45 p.m.




